B-ALI Bronchial Air Liquid Interface Media Kit, a guaranteed 3D in vitro model for respiratory research
By By Sorin Damian, George Klarmann and Marjorie Smithhisler, Lonza Walkersville, Inc
Sunday, 10 October, 2010
Introduction
The airway epithelium protects the airway from injury. This physical barrier is maintained by tight junctions between adjacent airway cells, and is reinforced by the secretion of mucus in order to trap pathogens, particulates and toxins. Though human airway epithelial primary cells and cell lines are well studied, traditional monolayer cell culture methods are limiting, due to submersion of the cells in culture medium. The Clonetics B-ALI Bronchial Air Liquid Interface Medium BulletKit provides a model system to investigate bronchial epithelial cells in a more physiologically relevant way.
The B-ALI System is a functional reconstitution of the airway mucosa in a bi-compartmental in vitro model, where primary human cells are grown on a suspended membrane and fed initially from both apical and basal chambers. Once a monolayer is established, the cells are fed only from the basal chamber while the apical chamber is exposed to air. The air-liquid interface (ALI) model reproduces the in vivo distribution of the airway lining where the epithelial cells face the airway lumen, and the basal pole of the cells is attached to the filter membrane. The epithelial cells attach to the membrane and form a tight, polarized multilayer. The differentiated culture contains a heterogeneous population of basal, secretory and ciliated cells. It is this heterogeneous culture of cells growing in a more physiologically relevant manner that makes the B-ALI System an ideal tool for the in vitro study of airway epithelium biology. This 3D model system more directly resembles the human airway compared to traditional bronchial epithelial cell culture methods which should facilitate better experimental design and results.
Methods and Materials
Clonetics Normal Human Tracheobronchial Epithelial Cells (NHBE) were screened for suitability in air-liquid interface culture. The screening protocol requires a short expansion mode in standard tissue culture conditions followed by airlift and differentiation on PET transwell inserts (Corning, catalog number 3470). Cultures in both the growth and differentiation phase of culture were kept at 37°C in humidified, 5% CO2 and 95% air. NHBE from Lonza (CC-2540) were thawed in B-ALI Growth Medium on standard T-75 tissue culture flasks at a density of 500,000 live cells per flask. After 3 days in culture (Fig. 1A) cells were trypsinized and replated in B-ALI Growth Medium on collagen-coated PET filter inserts at a density of 50,000 live cells/well (in 24-well filter plate format). Cells were fed for 3 more days with 100 µl B-ALI Growth Medium in the apical chamber and 500 µl in the basal chamber. By day 3 the NHBE monolayer was airlifted by removing the media from the apical chamber and feeding the cells only from the basal chamber with B-ALI Differentiation Medium containing B-ALI Inducer as per manufacturer instructions.
The differentiated phenotype of the cells was assessed between 7 and 30 days during airlift. For barrier function assessment, trans-epithelial electrical resistance (TEER) was measured at various time points using the EVOM Voltohmmeter (World Precision Instruments, Sarasota, FL). Secretory phenotype was assessed by measuring mucin secretion using direct staining with Alcian Blue (8GX, MPBiologicals, catalog number 152624). Ciliogenesis was evaluated by the appearance of the β-tubulin marker using an anti-β-tubulin-FITC antibody, clone TUB2.1 (Sigma, catalog number 2043). Scanning electron microscope (SEM) pictures were taken at M. E. Taylor Engineering Inc., Rockville, MD, 20855. Histological sections and confocal microscope pictures were taken in the Critical Care Medicine Department Lab, Clinical Center, National Institutes of Health in Bethesda, Maryland.
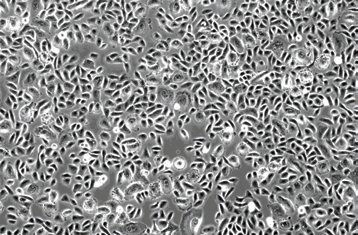 
Figure 1: (A) NHBE phenotype by day 3 in expansion mode (non-coated tissue culture plastic, growth media; 10X); (B) 3D aspect of the apical pole of the confluent monolayer at the beginning of the airlift phase (10X). |
Results and discussion
Early passages of normal human tracheobronchiolar epithelial cells (NHBE) will differentiate in vitro into airway epithelium and elicit the major functions of the in vivo human airway epithelium. The same functionality was reported by previous work.2 This report addresses the development of an accelerated growth and differentiation protocol using materials easily available, including pre-screened NHBE cells. Different lots of NHBE cells were screened for their ability to function in the ALI model system. Some lot-to-lot variation was noted, which is why Lonza provides B-ALI Pre-screened Lots of NHBE cells (CC-2540). Pre-screened NHBE lots are available at no additional charge, and will be identified after calling technical support. A comparison of NHBE monolayer culture and airlift culture phenotype is shown in Fig. 1.
|
|
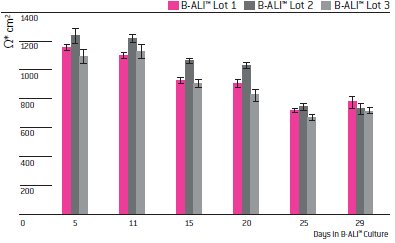
Confidence in the barrier function of these cells in airlift phase was supported by TEER readings (Fig. 2). The high resistance observed at both early (day 5) and late (day 29) times in ALI culture confirm that the cells form and maintain a tight barrier throughout the ALI culture period.
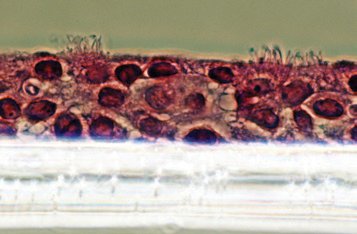
Immunofluorescence indicates strong expression of multiple tight junction proteins by NHBE cells when using the B-ALI System, which demonstrates the establishment of polarized epithelium. The fully differentiated cells in the air-liquid interface model offers the opportunity to expand those kinds of studies with simple and accessible endpoints, like assessment of structural tight junction protein integrity (e.g., ZO-1, occludin, cadherin, etc.) which can be easily disrupted by infective agents. Polarization is also confirmed by the appearance of intra-ciliary tubulin filaments within approximately 20 days in culture (Figs. 3A and 3B). The amount of cilia is variable from donor to donor, but very obvious around 20 days after airlift. Differentiated cultures will reach over 60 - 70% cilia density. (Fig. 3C). A cross sectional analysis of the differentiated NHBE in ALI culture clearly reveals the cilia on the apical surface, a stratified cell layer and the filter surface (Fig. 3D). These cells are suitable for inhibition studies of the DUOX antimicrobial system after Pseudomonas bacterial infection1 or for viral infection studies such as with rhinovirus and respiratory syncytial virus, the latter of which injures ciliated cells.6, 8
|
|
|
|
|
|
|
|
|
|
|
Figure 3: (A) and (B) Emerging cilia assessed by SEM (day 20 after airlift). (C) β-tubulin staining, day 25 in ALI; 10X mag, fluorescent microscopy; (D) Morphologic features of NHBE cells differentiated into mucociliary phenotype; histological preparation of a culture section (20X); (E) Tight junction proteins (ZO-1) and cilia (β-tubulin) are well developed 30 days after airlift. |
Secreted airway surface liquid (ASL) is visible from the first week after ALI. ASL is a protective liquid film necessary for the mucociliary clearance; however, the correlation between ASL volume and composition and the mechanisms by which mucin secretion rate is controlled is still poorly understood.4 Mucin secretion by NHBE cells in the B-ALI System was verified by Alcian Blue Staining (Fig. 4) at day 20. Mucin production requires PKC activation which suggests a possible use of the B-ALI System for screening of PKC inhibitors.5 The amount and viscosity of the ASL varies from donor to donor, and it is easily sampled for multiple studies. The ASL contains a mucus component, antibacterial agents like lysozyme and lactotransferrin, cell debris shed during differentiation, ectoenzymes, cytokines and signaling molecules.7 A recent proteomics study found that the ASL secreted by NHBEs in ALI culture is quite similar in protein composition to human sputum.3
|
|
The Clonetics B-ALI Bronchial Air Liquid Interface Medium BulletKit provides scientists with a unique tool to investigate new areas of bronchial epithelial research in a more physiologically relevant way. Some of these include gene therapy studies, host defense, gene expression analysis, preclinical drug development including inhaled drug formulations, disease models, airborne toxicant studies, and bio-defense models. The B-ALI BulletKit promotes full differentiation of the airway epithelium expressed by the formation of a polarized epithelium with good barrier function (transepithelial resistance), secretory phenotype (mucin secretion) and ciliogenesis. By using an air-liquid interface bronchial model, the next generation tool of in vitro respiratory research, scientists can explore bronchial epithelial cell differentiation and apply therapies in novel ways.
References
1. Balázs Rada, Kristen Lekstrom, Sorin Damian, Corinne Dupuy and Thomas L. Leto. 2008. The Pseudomonas Toxin Pyocyanin Inhibits the Dual Oxidase-Based Antimicrobial System as It Imposes Oxidative Stress on Airway Epithelial Cells. J.Immunol., 181: 4883-4893.
2. Gray TE, Guzman K, Davis CW, Abdullah LH, Nettesheim P. Mucociliary differentiation of serially passaged normal human tracheobronchial epithelial cells. Am J Respir Cell Mol Biol. 1996 Jan;14(1): 104-112.
3. Kesimer, M., Kirkham, S., Pickles, R.J., Henderson, A. G., Alexis, N. E., DeMaria, G., Knight, D., Thornton, D. J., Sheehan, J. K. 2009 Tracheobronchial air-liquid interface cell culture: a model for innate mucosal defense of the upper airways? Am J Physiol Lung Cell Mol Physiol volume 296: pp L92-L100.
4. Knowles, MR, & Boucher, RC. (2002). Mucus clearance as a primary innate defense mechanism for mammalian airways. J. Clin. Invest., 109: 571-7.
5. Park JA, Crews AL, Lampe WR, Fang S, Park J, Adler KB. 2007. Protein kinase C δ regulates airway mucin secretion via phosphorylation of MARCKS protein. Am J Pathol. 2007 Dec;171(6): 1822-30.
6. Sajjan, U, Wang, Q., Zhao, Y., Gruenert, D.C., Hershenson, M.B., 2008. Rhinovirus disrupts the barrier function of polarized airway epithelial cells. Am J Respir Crit Care Med volume 178: pp 1271-1281.
7. Tarran, R. 2004. Regulation of Airway Surface Liquid Volume and Mucus Transport by Active Ion Transport. Proc. Amer. Thor. Soc 1: 42-46.
8. Tristram, D. A., Hicks, W. Jr., Hard, R., 1998. Respiratory syncytial virus and human bronchial epithelium. Arch Otolaryngol Head Neck Surg volume 124: pp 777-783.
Are lab gloves leading scientists to overestimate microplastics?
Nitrile and latex gloves worn by scientists measuring microplastics may lead to a potential...
Newly created antivenom protects against 19 deadly snakes
By using antibodies from a human donor with a self-induced hyper-immunity to snake venom, US...
Antimicrobial coating for sanitary fabrics inspired by mussels
The innovative material fights against the spread of pathogens and antimicrobial resistance,...