100% human skin graft developed
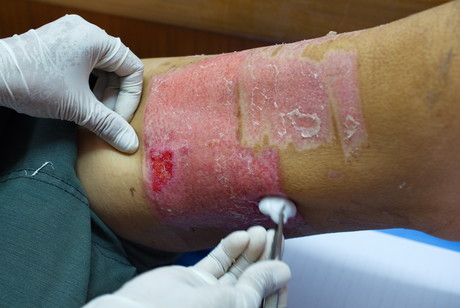
Singaporean researchers have made a skin graft cell culture using only human cells, which could be used to provide safer treatment for severe burns and other skin conditions in the future.
Skin grafting procedures have improved greatly in recent years, going as far as restoring 90% of the body surface of patients with severe skin wounds or burns. For such treatments, skin cells known as keratinocytes are collected from the patient and grown in cell culture in the laboratory to form a larger patch of tissue, which can then be grafted onto the wounds.
Often cells derived from mice are added to the culture to support tissue growth, but this human/mouse cell mix exposes patients to the risk of infections and adverse immune reactions; as such, the animal-derived products and biological agents used in the culture system are considered high-risk under Good Manufacturing Practice (GMP). Regulatory agencies, such as the US Food and Drug Administration (FDA), have classified such cultured products as xenografts, which are approved only for treatment of severe burns (above 30% of total body surface area) or for compassionate use.
Seeking a safer treatment option, researchers from Duke-NUS Medical School found a type of protein in the human body that can be used as a substitute for mouse cells. Led by Professor Karl Tryggvason, who also has ties to Sweden’s Karolinska Instititet, the team found that two specific variants of proteins called laminins, LN-511 and LN-421, can support the growth of human keratinocytes in a similar way to mouse cells.
“Laminins have been transforming cell biology and are known to maintain stem cells and tissues architecture and function in a way that mimics the situation in the human body,” Prof Tryggvason said. “The laminins play an important role in several human diseases, such as those of skin.
“Our method of using biologically relevant laminins in their pure forms to develop a fully human cell culture system for growing skin keratinocytes in the laboratory is a first and is likely to translate into novel treatments for many different skin disorders and wounds.”
Described in the journal Nature Communications, the team’s finding allowed them to completely remove the use of mouse cells and create a fully human, animal-free cell culture system for skin grafting. They then demonstrated that skin tissue obtained using this method could be successfully grafted onto mice, which they say is an important step forward for regenerative medicine.
“This new method provides a robust yet safer system for our burn patients,” said Dr Alvin Chua, co-lead author of the study from Singapore General Hospital and Duke-NUS Medical School. “More importantly, it sets the stage for a cell culture platform for other regenerative medicine applications — these include the cultivation of cells from other surface tissues of the body, such as the cornea or oral mucosa.”
Proposed Australian trial eyes up blood testing for Alzheimer's
Utilising networks of GPs across three states, a large-scale study intends on combining digital...
Applications open for $300K pandemic therapeutics fellowships
Applications are now open for the Cumming Global Centre for Pandemic Therapeutics' inaugural...
CTA granted for CAR-T cell therapy for multiple myeloma
The Therapeutic Goods Administration has granted Clinical Trial Approval for KMCAR T-cell...




